|
| |
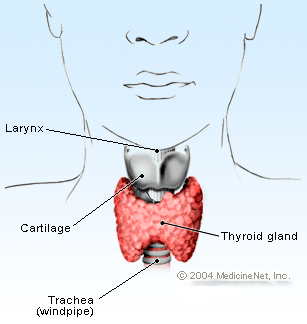
The thyroid gland is located on the front part of the neck below the thyroid
cartilage (Adam's apple). The gland produces thyroid hormones, which regulate
metabolic rate (how fast calories are consumed to produce energy). Thyroid
hormones are important in regulating body energy, body temperature, the body's
use of other hormones and vitamins, and the growth and maturation of body
tissues.
Diseases of the thyroid gland can result in either production of too much
(overactive thyroid disease or hyperthyroidism),
too little (underactive thyroid disease orhypothyroidism)
thyroid hormone, thyroid
nodules, and/or goiter. Thyroid problems are much more common in women than
in men.
-
Production of thyroid hormones:The process of
hormone synthesis begins in a part of the brain called the hypothalamus. The
hypothalamus releases thyrotropin-releasing hormone (TRH). The TRH travels
through the venous plexus located in the pituitary stalk to the pituitary
gland, also in the brain. In response, the pituitary gland then releases
thyroid-stimulating hormone (TSH, also called thyrotropin) into the blood.
The TSH travels to the thyroid gland and stimulates the thyroid to produce
the two thyroid hormones, L-thyroxine (T4) and triiodothyronine (T3). The
thyroid gland also needs adequate amounts of dietary iodine to be able to
produce T4 and T3, the molecules of which contain four and three atoms of
iodine, respectively.
-
Regulation of thyroid hormone production: To
prevent the overproduction or underproduction of thyroid hormones, the
pituitary gland senses how much hormone is in the blood and adjust the
production of hormones accordingly. For example, when there is too much
thyroid hormone in the blood, TRH and TSH production are both decreased. The
sum effect of this is to decrease the amount of TSH released from the
pituitary gland and to reduce production of thyroid hormones from the
thyroid gland to restore the amount of thyroid hormone in the blood to
normal. Defects in these regulatory pathways rarely may result in
hypothyroidism (underactive thyroid problem) or hyperthyroidism (overactive
thyroid problem). The most common cause of hypothyroidism and
hyperthyroidism occurs due to problems within the thyroid and not the
regulatory system.
-
Thyroid goiter: Thyroid
goiter is any enlargement of the thyroid that can occur with hyperthyroidism
or hypothyroidism but also with benign and malignant (cancerous) nodules.
Worldwide, the most common cause of goiter is iodine deficiency. Although it
used to be very common in the U.S., it is now less common with the use of
iodized salt. Multiple nodules in the thyroid are very common, but only
about 5% of the nodules are a thyroid
cancer. Thyroid cancer rates have been increasing steadily by about 6%
every year for more than 20 years. It is one of the few cancers whose rate
is increasing and whose very low rate of mortality is also rising with time.
Although radiation exposure as a child can increase the risk of thyroid
cancer, we do not know why the overall rate has been increasing. Thyroid
cancer is diagnosed after a thyroidultrasound exam
and a needle aspiration biopsy of the nodule.
Thyroid Problems Symptoms
Symptoms of thyroid problems depends on the age of the person and the exact
problem with the thyroid. For example, some symptoms of hypothyroidism in
children include:
Symptoms similar to adult symptoms
Excessive fatigue
Poor growth
Poor school performance
Symptoms of hypothyroidism in adults include:
Easy fatigue, exhaustion
Poor tolerance to cold temperatures
Constipation
Carpal tunnel syndrome (pain at the wrists and numbness of the hands)
Some of the symptoms of hyperthyroidism in adults include:
Insomnia
Hand tremors
Nervousness
How common is thyroid disease?
Thyroid disease is more common than diabetes or heart disease. Thyroid
disease is a fact of life for as many as 30 million Americans – and more than
half of those people remain undiagnosed. Women are 5 times more likely than men
to suffer from hypothyroidism (when the gland is not producing enough thyroid
hormone). Aging is just one risk factor for hypothyroidism.
hide
How important is my thyroid in my overall well-being?
The thyroid gland produces thyroid hormone, which controls virtually every
cell, tissue, and organ in the body. If your thyroid is not functioning
properly, it can produce too much thyroid hormone, which causes the body’s
systems to speed up – this is called hyperthyroidism; or it can create too
little thyroid hormone, which causes the body’s systems to slow down – this is
called hypothyroidism. If your thyroid gland isn’t working properly, neither
will you.
Untreated thyroid disease may lead to elevated cholesterol levels and subsequent
heart disease, as well as infertility and osteoporosis. Research also shows that
there is a strong genetic link between thyroid disease and other autoimmune
diseases, including types of diabetes, arthritis, and anemia.
hide
How do you know if you have a thyroid problem?
First, understand how to recognize the symptoms and risk factors of thyroid
disease. Since many symptoms may be hidden, the best way to know for sure is to
ask your doctor for a TSH (thyroid-stimulating hormone test), a simple blood
test to verify your thyroid gland’s condition. Also, take a minute and perform a
self “Neck Check. Because thyroid disease often runs in families, examinations
of your family members may reveal other individuals with thyroid problems.
hide
Who should have a TSH test?
Individuals over the age of 60 and those who have symptoms or the risk
factors associated with thyroid disease should talk to their doctor about
undergoing a TSH test.
hide
What causes hypothyroidism?
Hypothyroidism occurs when the thyroid gland does not produce enough thyroid
hormone. The most common cause of hypothyroidism is an autoimmune disease
called Hashimoto’s thyroiditis, in which the body’s immune system attacks the
thyroid. Hypothyroidism can also be caused by some treatments of hyperthyroidism
because the remaining active thyroid cells cannot produce enough thyroid
hormone. In addition, hypothyroidism can be caused by certain medicines such as
lithium, iodine, and amiodarone. Hypothyroidism can temporarily arise after
pregnancy or if the thyroid is inflamed due to a viral infection. This disease
can also be present at birth and runs in families.
hide
What can affect my thyroid disease treatment results?
To reach optimal treatment results, it is important to take your medicine as
instructed by your doctor. Do not stop taking your thyroid medicine, even if you
feel better, without talking to your doctor first. It is important to stay on
the exact dose and brand of medicine your doctor prescribes to help avoid any
variations in your thyroid hormone levels. Thyroid hormone imbalance can result
from untreated thyroid disease, or from over- or under-treatment. In addition,
various medicines and supplements may affect the absorption of thyroid hormone;
therefore, you should talk to your doctor about any medicines and supplements
you are taking and about the best time of day to take your thyroid medicine if
you are taking other medicines or supplements.
hide
What is radioiodine therapy?
If you have an overactive thyroid gland or have been diagnosed with thyroid
cancer, your endocrinologist may prescribe radioactive iodine (radioiodine) as
part of your overall treatment. You, your family, and your coworkers may have
some questions about this therapy.
hide
How is radioiodine therapy used to treat hyperthyroidism?
Before the development of current treatment options, the death rate from
severehyperthyroidism was as high as 50%. Now several effective treatments (antithyroid
drugs, surgery, and radioiodine) are available, and death from hyperthyroidism
is rare. Deciding which treatment is best depends on what caused the
hyperthyroidism, its severity, and other conditions present. Endocrinologists
are experienced in the management of thyroid diseases and can confidently
diagnose the cause of hyperthyroidism and prescribe and manage the best
treatment program for each patient.
Thousands of patients have received radioiodine treatment, including former
President of the United States George H. W. Bush and his wife, Barbara. The
treatment appears to be a very safe, simple, and reliably effective one. Because
of this, it is considered by most thyroid specialists in the United States to be
the treatment of choice for hyperthyroidism cases caused by overproduction of
thyroid hormones.
Radioactive iodine is given by mouth, usually in capsule form, and is quickly
absorbed from the bowel. It then enters the thyroid cells from the bloodstream
and gradually destroys them. Although the radioactivity from this treatment
remains in the thyroid for some time, it is largely eliminated from the rest of
the body within a few days. Its effect on the thyroid gland usually takes
between 1 and 3 months to develop, and maximal benefit is usually noted within 3
to 6 months.
It is not possible to eliminate “just the right amount” of the diseased thyroid
gland, since radioiodine eventually damages all thyroid cells. Therefore, most
endocrinologists strive to completely destroy the diseased thyroid gland with a
single dose of radioiodine. This results in the intentional development of an
underactive thyroid state (hypothyroidism), which is easily, predictably and
inexpensively corrected by lifelong daily use of oral thyroid hormone
replacement therapy. Although every effort is made to calculate the correct dose
of radioiodine for each patient, not every treatment will successfully correct
the hyperthyroidism, particularly if the goiter is quite large and a second dose
of radioactive iodine is occasionally needed.
hide
How is radioiodine therapy used for the treatment of thyroid cancer?
The two most common types of thyroid cancer (papillary and follicular) can
usually be treated with radioiodine because the cells are able to take up some
iodine. Radioiodine is used in treating thyroid cancer in the following two
general situations:
AFTER REMOVAL OF THE THYROID- An experienced thyroid surgeon can remove most of
the thyroid with a very low risk of surgical complications. Radioiodine can be
used to destroy the remainder of the thyroid gland, which might harbor
additional microscopic clusters of cancer cells. This is called radioiodine
remnant ablation. It is also used to treat thyroid cancer that has spread beyond
the thyroid gland. In this case, when thyroid cancer is definitely being treated
it is called radioactive iodine therapy. Elevated TSH levels are required in
order to adequately stimulate normal or cancerous cells to pick up enough
radioiodine for the treatment to be effective. This can be accomplished by
either not taking replacement thyroid hormone for several weeks after surgery or
by getting synthetic TSH (recombinant human thyrotropin) injections. Synthetic
TSH is FDA- approved for radioiodine remnant ablation, but not for treating
thyroid cancer that has already spread. This treatment significantly reduces the
possibility of recurrent cancer in whatever thyroid tissue is left and also
improves the ability to detect and treat any future cancer recurrences that
might develop.
DURING FOLLOW-UP- Patients with residual thyroid cancer or cancer that has
spread to regions outside of the neck can undergo a scan with a test amount of
radioiodine. Scanning with radioiodine helps to determine the extent of
“persistent” or “recurrent” thyroid cancer, whether it may respond to additional
doses of radioactive iodine, and how much radioactive iodine to use for
treatment. If any iodine is concentrated in the areas of the thyroid cancer,
another dose of radioiodine can be given to try to destroy the tumor. This
treatment is safe, well tolerated, and has successfully treated many cases of
thyroid cancer even after the tumor has spread.
All patients with thyroid cancer should have regular follow-up examinations by
an endocrinologist. Additional doses of radioactive iodine may be recommended if
thyroid cancer remains (which is called “persistent”) or reappears later (which
is called “recurrent”). Your thyroid hormone replacement therapy will need to be
stopped long enough to allow you to become hypothyroid, so that maximum response
to the treatment will occur.
hide
What happens to the radioiodine after a treatment?
Since surgery removes the vast majority of thyroid tissue, much of the
radioiodine will not be absorbed and will leave the body primarily through the
urine. Small amounts will also be excreted in saliva, sweat, tears, vaginal
secretions, and feces. Nearly all the radioactive iodine will leave the body
during the first 2 days after the dose has been given.
hide
What about breast-feeding during treatment?
Radioactive iodine treatment should never be given to a pregnant woman!
Small amounts of radioactive iodine will also be excreted in breast milk. Since
radioiodine could permanently damage the infant’s thyroid, breast-feeding is not
allowed. If radioiodine is inadvertently administered to a woman who is
subsequently discovered to be pregnant, the advisability of terminating the
pregnancy should be discussed with the patient’s obstetrician and
endocrinologist. Therefore, prior to administering diagnostic or therapeutic
radioiodine treatment, pregnancy testing is mandatory whenever pregnancy is
possible.
hide
Are future pregnancies possible?
For safety’s sake, males are advised to avoid fathering a child for several
months. Females are advised to postpone pregnancy for six or so months after
radioiodine treatment. Women are advised to wait longer to help stabilize their
thyroid status before conception. Even though the amount of radioactivity
retained may be small and there is no medical proof of an actual risk from
radioiodine treatment, there is a theoretical risk to a developing fetus. Such
precautions essentially eliminate direct fetal exposure to radioactivity, and
markedly reduce the possibility of conception with sperm that might
theoretically have been damaged by exposure to radioiodine. You may need to
contact your physician for guidance about methods of contraception.
Regulations regarding the use of radioiodine therapy are made by the US Nuclear
Regulatory Commission (NRC). Physicians and hospitals that administer this
therapy must have a license to administer radioiodine, and must adhere to
stringent regulations regarding its use. If you have any questions before or
after receiving your treatment, please do not hesitate to contact your physician
or your hospital radiation safety officer for clarification.
Click here to learn more about pregnancy and thyroid.
hide
Is hospitalization necessary for treatment with radioiodine?
Treatment for hyperthyroidism is almost always done on an outpatient basis,
because the dose required is relatively small in comparison with the doses
typically used for treatment of thyroid cancer. If you have to take a larger
dose of radioiodine for treatment of thyroid cancer, you may need to be admitted
to the hospital for several days depending on the amount of radioiodine
administered, your living environment, state of residence, or local practice
patterns.
If you require hospitalization, your hospital room will have frequently handled
items (such as the television control, table, phone, faucet handles, etc),
covered with protective material, and the floor will be partially covered. These
precautions are designed to prevent the radioactive iodine from contaminating
those items that will be reused by other patients after your dismissal from the
hospital. To limit the contamination of your personal items, you should bring a
minimal amount of belongings for your stay. All items will be monitored at your
dismissal. Clothing should be limited to what you wear when you are admitted.
You should use hospital gowns during your stay. You may want to bring disposable
items like magazines and newspapers, but important or durable items like
hardback books, work papers, and craft items should be left at home. Check with
your endocrinologist about any other issues.
hide
What are some recommendations for the reduction of exposure to others after
treatment?
Use private toilet facilities, if possible; flush twice after each use.
Bathe daily and wash hands frequently.
Drink normal amount of fluids.
Use disposable eating utensils or wash your utensils separately from others.
Sleep alone and avoid prolonged intimate contact.
Launder your linens, towels, and clothes daily at home, separately from others.
No special cleaning of the washing machine is required between loads. This is
because the radioiodine administered is water soluble.
Do not prepare food for others that requires prolonged handling with bare hands
(such as mixing a meat loaf or kneading bread)
Brief periods of close contact, such as handshaking and hugging, are permitted.
Your endocrinologist or radiation safety officer may recommend continued
precautions for up to several weeks after treatment, depending on the amount of
radioactivity administered and retained by your body. Patients receiving
radioactive iodine should also carry information about their treatment with them
in order to fully inform authorities who are in charge of screening for
radioactive materials in public areas such as airports and subways.
hide
( Courtesy: http://www.emedicinehealth.com,
http://www.thyroid.org/ )
Articles:
More Articles:
| |
|